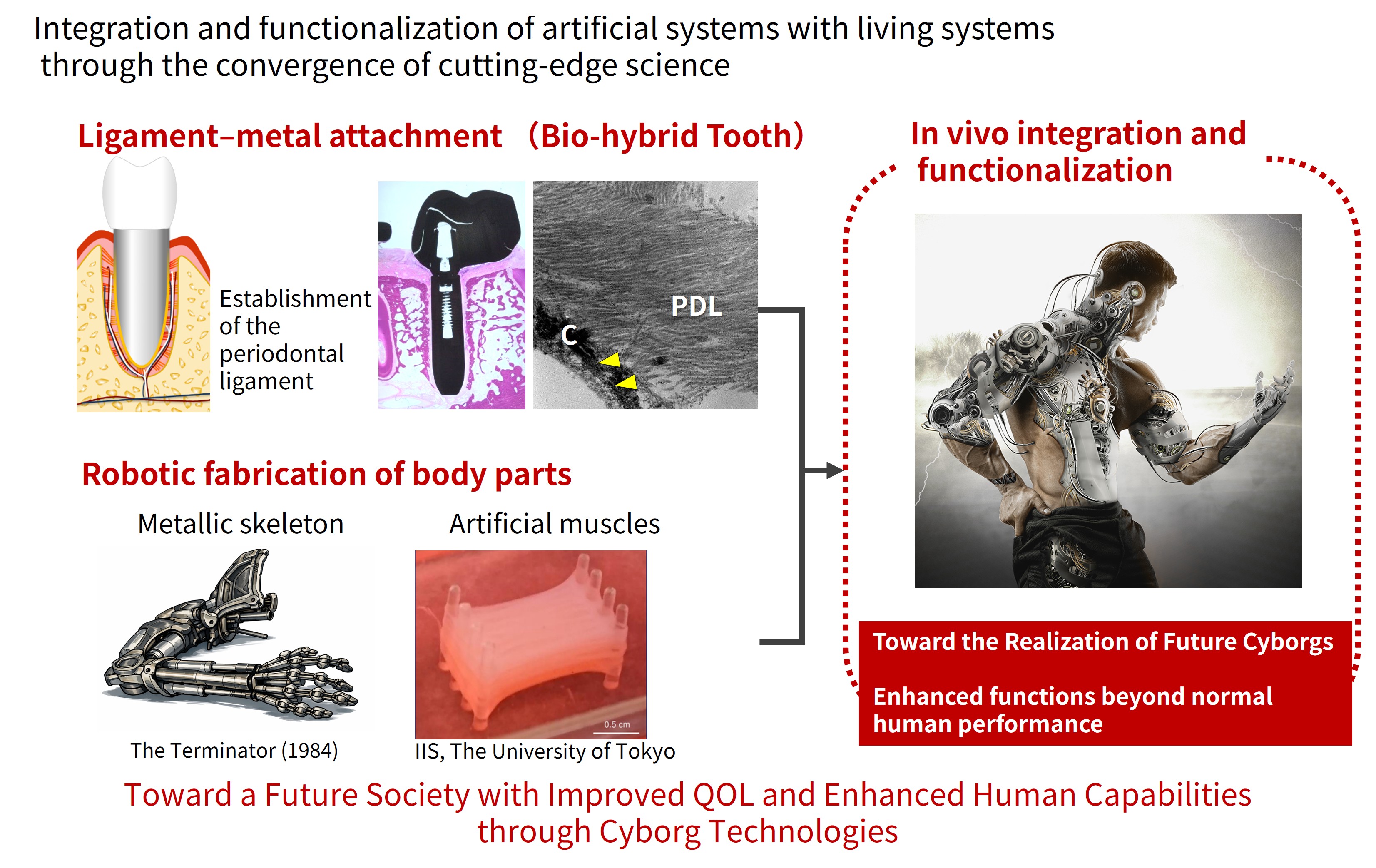
4 OrganTech's Challenge (2)
- Hybridizing Living Tissue and Artificial Materials

Ph.D. in Science from Kyushu University Graduate School. Has held positions including Professor at Tokyo University of Science, Team Leader at RIKEN BDR, and others. Currently Visiting Professor at Tokyo Dental College and Visiting Senior Scientist at RIKEN. Founded OrganTech in 2008 and became Chairman in 2024. View full profile >
The regeneration of a functional tooth (described in Chapter 3) opened the door to the future of organ regeneration. However, in order to realize this as a clinical therapy, we encountered two major barriers.
One of them was the time required for tooth eruption. Normally, permanent teeth require approximately five years from the tooth germ stage until the tooth fully erupts. For example, if a patient were to undergo regenerative therapy in which a regenerated tooth germ is transplanted at a dental clinic and be told, "Your tooth will erupt in five years," it raises the question of whether this could realistically function as a clinical treatment. We considered whether this period could be shortened to six months or one year, but as discussed in the concept presented in the book "Elephant Time, Mouse Time" by Tatsuo Motokawa, the biological clock governing developmental timing has not yet been altered.
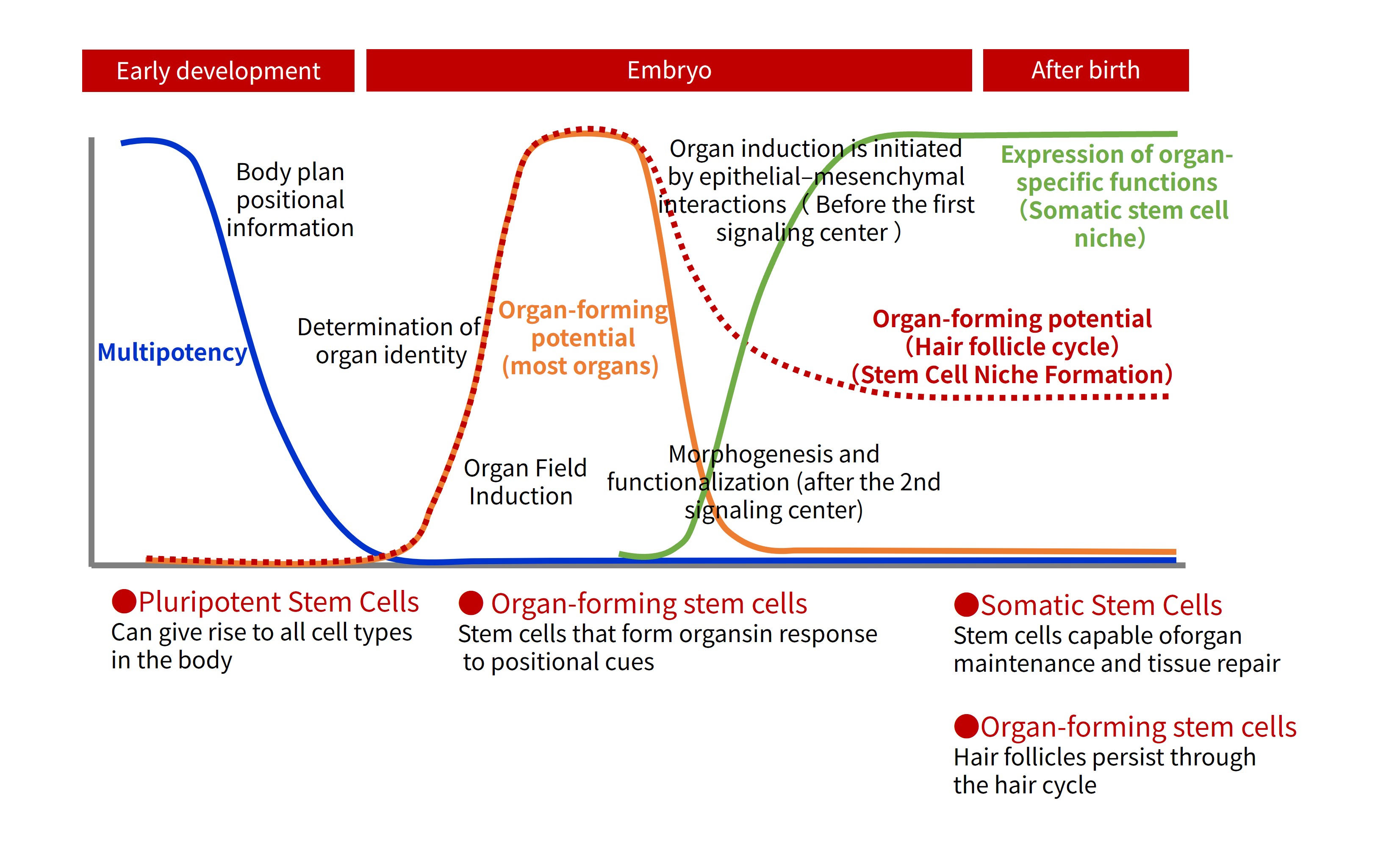
Another major challenge was that the stem cells capable of regenerating the tooth germ, which is the organ primordium of the tooth, exist only during the fetal stage. Organ primordia - the "seeds" of organs - are induced during fetal development through epithelial-mesenchymal interactions between two types of stem cells that possess organ-inductive capacity: Epithelial stem cells and Mesenchymal stem cells (MSCs).
Once an organ has been induced from the organ primordium before birth, these organ-inductive stem cells transform into somatic stem cells that repair tissues and maintain organ function (Figure 1). As a result, when an organ becomes dysfunctional due to injury or disease, the only available treatment is often organ transplantation. Therefore, tooth germ-forming cells required for tooth regeneration cannot be harvested once a person is born and permanent teeth begin to erupt.
We successfully demonstrated proof of concept for functional tooth regeneration, which was a highly significant achievement in biomedical science. However, two major barriers still stood in the way of practical application. Fortunately, our research on tooth regeneration was widely accepted by scientific communities in developmental biology, regenerative medicine, dentistry, and medicine around the world. We were invited to many international conferences and had numerous opportunities to present our findings.
During these discussions, dental researchers from around the world repeatedly told us: "Regenerating an entire tooth is remarkable. But if a periodontal ligament could be regenerated around current osseointegrated implants, that itself would represent functional tooth regeneration."
At that moment, a new path toward the practical application of tooth regeneration opened before us.
Modern dental implant therapy restores not only occlusal function but also aesthetics, without damaging adjacent healthy teeth. Moreover, because implants can stably replace occlusal function over the long term, they have developed into a treatment that has fundamentally transformed dental therapy for tooth loss (as described in Chapter 2). However, osseointegrated implants are directly integrated with the alveolar bone, and therefore lack the periodontal ligament that connects the tooth root to the alveolar bone in a natural tooth (Figure 2, Chapter 1 and Chapter 2).
The periodontal ligament performs many important physiological functions, including:
- ・Shock absorption of occlusal forces during mastication
- ・Sensory perception
- ・Defense against infection
- ・Tooth mobility and orthodontic movement
Furthermore, the absence of periodontal ligament tissues creates several clinical and social issues. For example:
- ・Implants cannot be applied to young patients whose jaws are still growing.
- ・In an aging society, if a bedridden elderly patient with implants requires extraction, the procedure may be difficult, raising concerns about systemic infections.
For these reasons, there has been strong demand for research and development aimed at advancing implant therapy toward a treatment that possesses functions closer to those of natural teeth.
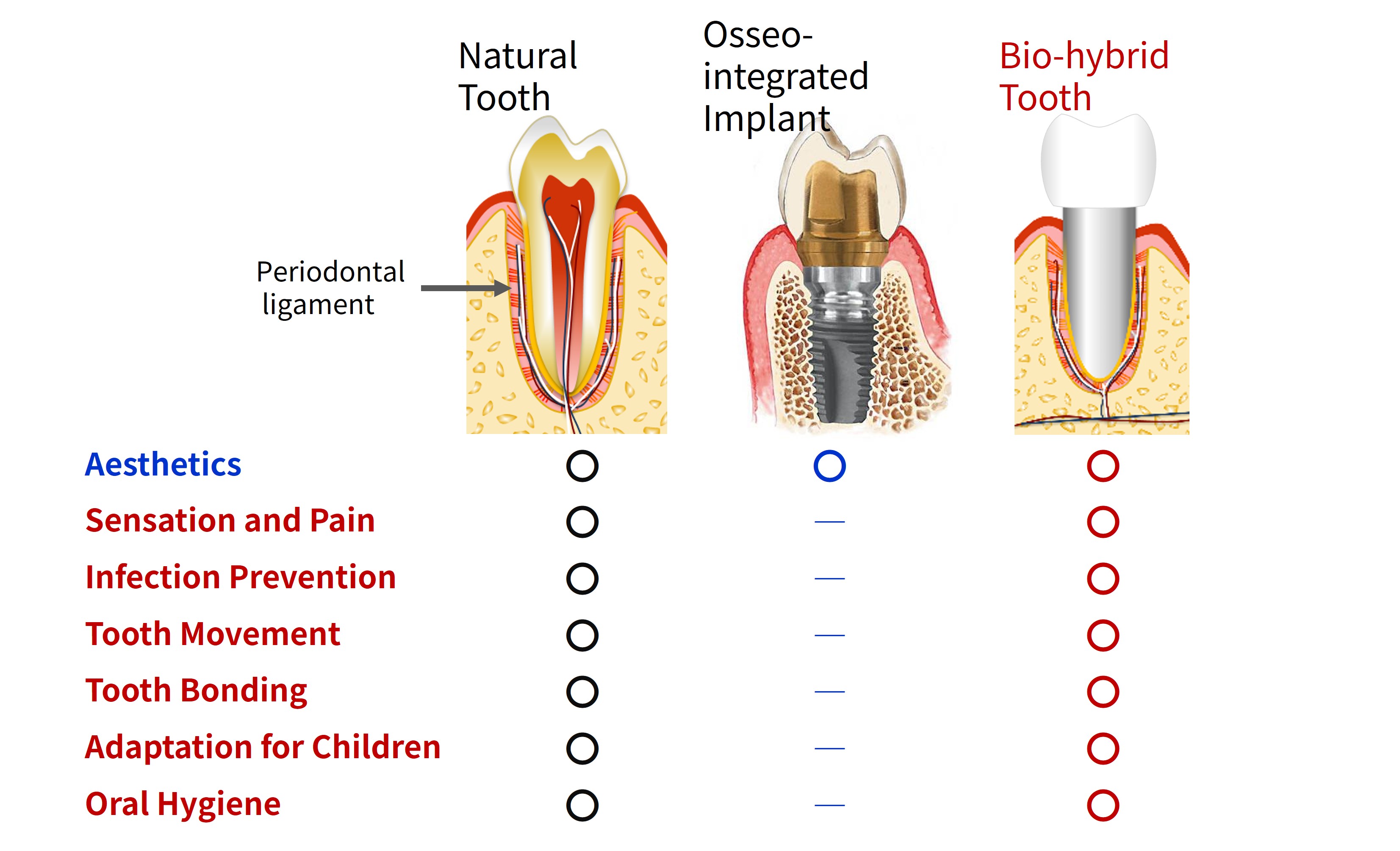
If a periodontal ligament could be added to a dental implant, thereby restoring functions equivalent to those of a natural tooth, the implant could become a reinforced tooth made of metal that does not develop dental caries. Such a tooth could potentially serve as a "third dentition," following the primary teeth and permanent teeth.
A fusion of living tissue and metal - a concept reminiscent of a cyborg (Figure 3). Thus, our new challenge began.