Chapter
2 Treatment Options After Tooth Loss
— The Current State and Limitations of Dental Implants
2 Treatment Options After Tooth Loss
— The Current State and Limitations of Dental Implants
Last updated: February 13, 2026

Takashi Tsuji, Ph.D. Chairman of the Board / Founder
Ph.D. in Science from Kyushu University Graduate School. Has held positions including Professor at Tokyo University of Science, Team Leader at RIKEN BDR, and others. Currently Visiting Professor at Tokyo Dental College and Visiting Senior Scientist at RIKEN. Founded OrganTech in 2008 and became Chairman in 2024. View full profile >
Ph.D. in Science from Kyushu University Graduate School. Has held positions including Professor at Tokyo University of Science, Team Leader at RIKEN BDR, and others. Currently Visiting Professor at Tokyo Dental College and Visiting Senior Scientist at RIKEN. Founded OrganTech in 2008 and became Chairman in 2024. View full profile >
Tooth loss has a profound impact on essential functions such as chewing and eating. Therefore, conventional dental treatments have focused on restoring occlusal function through functional replacement using artificial materials, including removable dentures, fixed bridges, and dental implants (Figure 1).
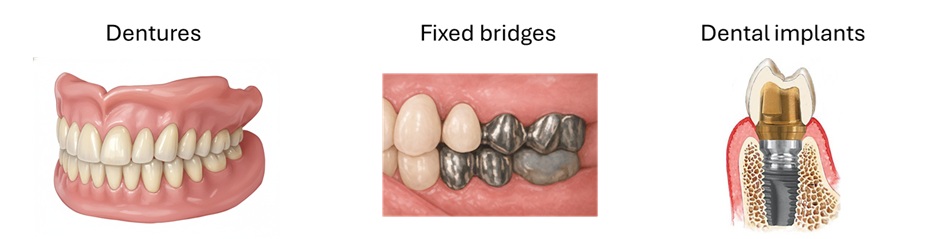
Figure 1 Artificial Dental Treatment Options for Tooth Loss
The history of such restorative treatments is ancient. During the Sengoku period in Japan, wooden dentures used by Buddhist nuns have been documented, while in the fifth century BCE, wire-fixed bridges already existed (Figure 2). Furthermore, in the Maya civilization around the seventh century CE, implants made from mother-of-pearl were used, and remarkably, these demonstrated bone integration similar to modern dental implants (Figure 2). This long history of prosthetic tooth replacement clearly illustrates the fundamental importance of restoring occlusal function for human survival and quality of life. Although these artificial restorations successfully recover occlusal function, they also present inherent limitations. Removable dentures often suffer from insufficient stability, while fixed bridges require the preparation and reduction of adjacent natural teeth, which can compromise their structural integrity.
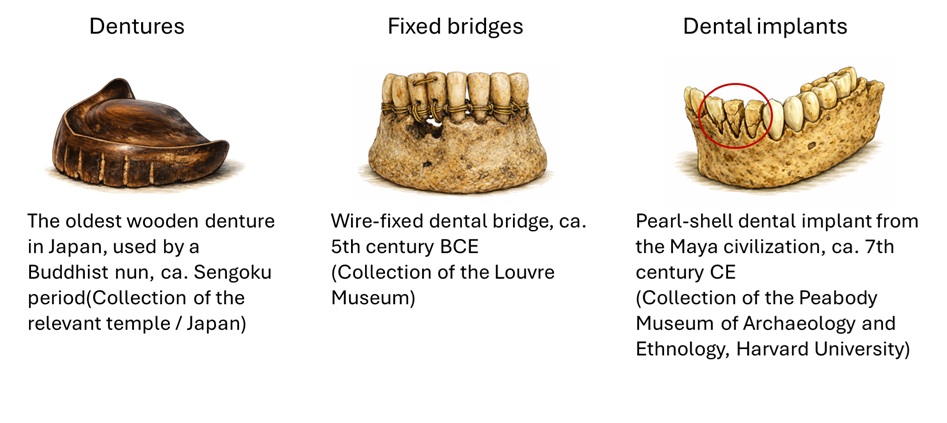
Figure 2 History of Dental Treatment for Tooth Loss
In the 1960s, osseointegrated dental implant therapy was developed using titanium implants that directly bond to the alveolar bone. Since then, continuous technological advancements have greatly improved implant design, materials, and clinical protocols. Contemporary dental implant therapy enables restoration of occlusal function and esthetics without damaging adjacent natural teeth, and provides long-term functional stability. As a result, it has fundamentally transformed the treatment paradigm for tooth loss.
However, while artificial material–based therapies are highly effective in restoring mechanical function and appearance, they are unable to recover the physiological functions inherent to the natural tooth. In dental implant therapy—currently regarded as the most advanced treatment for tooth loss—the implant is directly connected to the alveolar bone, and thus lacks the periodontal ligament that physiologically links the tooth root to surrounding bone (Figure 3). The periodontal ligament plays diverse and essential roles in tooth function, as discussed in Chapter 1. It acts as a shock absorber for occlusal forces during mastication, allows the ingress of blood vessels and nerves to mediate sensory perception and pain, facilitates immune defense against infection, and enables orthodontic and adaptive tooth movement. Consequently, dental implants inherently lack these critical biological functions provided by the periodontal tissues.
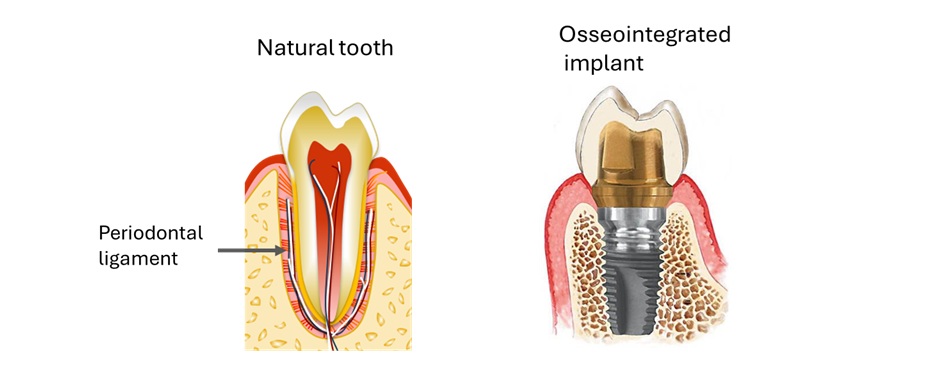
Figure 3 Periodontal Ligament in Natural Teeth and Implants
The absence of periodontal ligament tissue further limits the applicability of dental implants in young patients whose alveolar bone is still undergoing growth and remodeling. In addition, long-term physiological tooth movement associated with aging can result in occlusal disharmony, which is difficult to compensate for with rigid osseointegrated implants. Moreover, in an increasingly aging society, a significant clinical concern arises in bedridden elderly patients. When tooth extraction is required to maintain oral hygiene and prevent systemic infection, osseointegrated dental implants—lacking periodontal ligament and being firmly anchored to the alveolar bone—cannot be easily removed. This poses a serious risk for systemic infectious complications and represents an important public health issue.
At present, treatments for tooth loss—including dentures, bridges, and dental implants—play a crucial role in national health by restoring the ability to chew and eat, which lies at the core of a healthy society. With continued advances in science and biotechnology, there is growing expectation for biologically based therapies that go beyond mechanical replacement. In particular, regenerative approaches aiming to restore periodontal tissues—comprising cementum, periodontal ligament, and alveolar bone—may enable recovery of the physiological functions of the natural tooth and reestablishment of the functional occlusal system (Chapter 1).
* This article reflects research and development-stage information as of February 13, 2026, and does not represent finalized medical procedures or products.
** The illustrations on this page are images created based on historical materials.
