3 OrganTech's Challenge (1)
- Regenerating Teeth

Ph.D. in Science from Kyushu University Graduate School. Has held positions including Professor at Tokyo University of Science, Team Leader at RIKEN BDR, and others. Currently Visiting Professor at Tokyo Dental College and Visiting Senior Scientist at RIKEN. Founded OrganTech in 2008 and became Chairman in 2024. View full profile >
Many patients undergo dental treatment while hoping, “I want to regain my own tooth that was lost due to caries, trauma, or periodontal disease.” In a healthy and aging society, preventing tooth loss through dental care, as well as enhancing therapeutic options for tooth loss, represents a critical challenge for future dentistry.
In the 21st century, regenerative medicine using stem cells has advanced significantly. As examples of partial regeneration of dental tissues, regenerative therapies such as regeneration of the dental pulp for caries and regeneration of the periodontal ligament for periodontal disease have been developed. In contrast, a major goal in the treatment of tooth loss is the regeneration of the entire tooth. A tooth is a single “organ” composed of multiple cell types arranged in a precise three-dimensional configuration, and whole-tooth regeneration therefore means regeneration of an entire organ (Figure 1, Organ Regeneration). Although three-dimensional organ regeneration has been studied for several decades, technological development has not progressed sufficiently for any organ. Therefore, tooth regeneration has been expected to serve as a model case for organ regeneration.
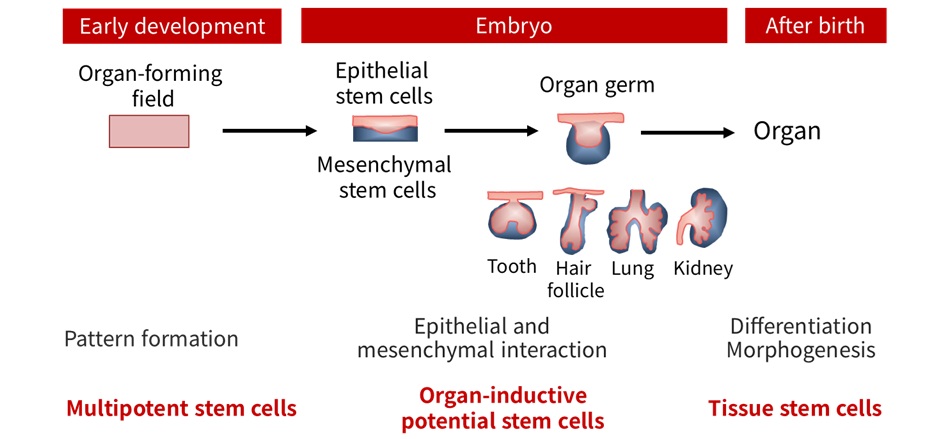
A tooth develops from the “tooth germ,” which is induced by interactions between epithelial stem cells and mesenchymal stem cells during the fetal period (Chapter 1, Organ Regeneration). Our initial challenge was to isolate these two types of stem cells with organ-inducing potential from fetal tissues and to develop cell manipulation techniques that would enable their proper three-dimensional arrangement to recapitulate normal tooth development. In the field of developmental biology, this had remained an unfinished technological challenge for more than 30 years (Organ Regeneration).
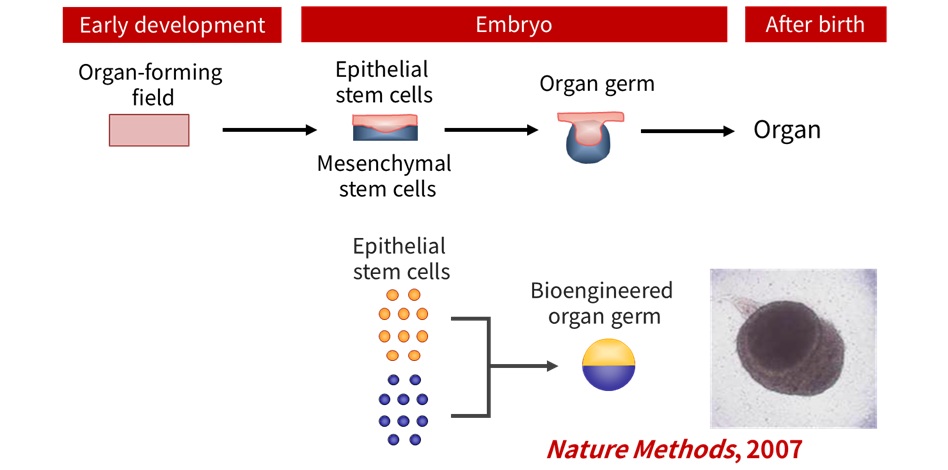
We undertook this challenge and repeated trial and error over many years. In 2007, we became the first in the world to develop the “organ germ method,” in which epithelial stem cells and mesenchymal stem cells are compartmentalized and arranged at high density to reproduce epithelial-mesenchymal interactions in vivo (Figure 2). This technology became the foundation for all subsequent organ regeneration research. The development of this method attracted worldwide attention as the first example of “whole-tooth regeneration,” and we received numerous invitations to deliver lectures, particularly in the dental field. However, at that time, we had only established a three-dimensional cell manipulation method to regenerate the tooth germ, and the regenerated tooth had not yet erupted, which made us uneasy about the excessive media attention. Moreover, many researchers pointed out, “Teeth erupt along the eruption pathway. Even if you transplant a regenerated tooth germ, it will not erupt without this pathway.” Nevertheless, we believed that regenerated tooth germs could erupt. With this conviction, we developed a new animal model and initiated another challenge.
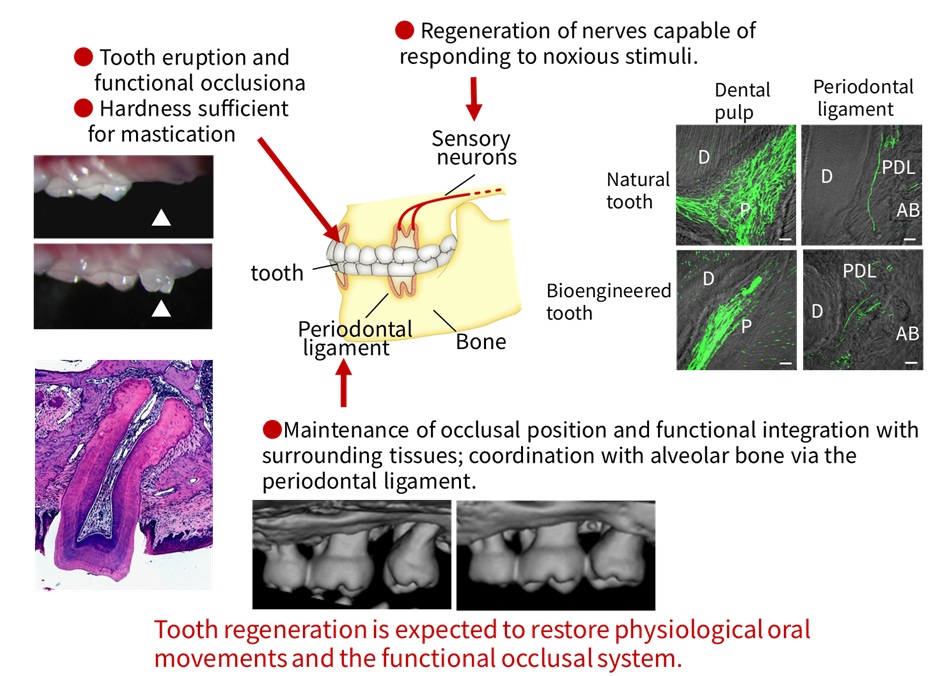
In 2009, we isolated the two types of stem cells from mouse fetal tooth germs, regenerated tooth germs using the organ germ method, and transplanted them into sites of tooth loss. We demonstrated that the regenerated teeth erupted and achieved occlusion (Figure 3). The regenerated teeth exhibited the same structure as a natural tooth and were connected to the alveolar bone via the periodontal ligament, forming occlusion with opposing teeth. Functional analysis of the periodontal ligament revealed that the regenerated teeth possessed the capacity for movement through bone remodeling in response to experimental orthodontic force. Furthermore, sensory nerves had infiltrated the periodontal ligament, and stimulation of the dental pulp or orthodontic force induced sensory responses in the medulla oblongata. These findings astonished researchers in the dental field, and we began receiving even more invitations for lectures from around the world.
These results demonstrated the potential to regenerate fully functional teeth indistinguishable from natural teeth. Using the organ germ method, we further demonstrated the functional regeneration of hair follicles, salivary glands, and lacrimal glands in vivo, paving the way for future organ regenerative medicine and making a significant global impact (Figure 4).

