5 OrganTech's Challenge (2-2)
- Integrating Implants with the Body Through the Periodontal Ligament

Ph.D. in Science from Kyushu University Graduate School. Has held positions including Professor at Tokyo University of Science, Team Leader at RIKEN BDR, and others. Currently Visiting Professor at Tokyo Dental College and Visiting Senior Scientist at RIKEN. Founded OrganTech in 2008 and became Chairman in 2024. View full profile >
The importance of the Periodontal ligament in tooth physiological function has long been recognized, and attempts to generate periodontal ligament tissue around oral implants have been investigated for many years. Various approaches have been explored, including coating implant surfaces with bioactive materials that induce periodontal ligament formation and seeding cells possessing periodontal ligament–forming capacity onto implant surfaces. However, no previous studies had successfully achieved the complete reconstruction of Periodontal tissues, including functional integration.
From the perspectives of developmental biology and regenerative medicine, we initiated fundamental research in 2009 using a mouse model to develop a “next-generation biohybrid implant” capable of conferring a periodontal ligament onto an implant fixture.
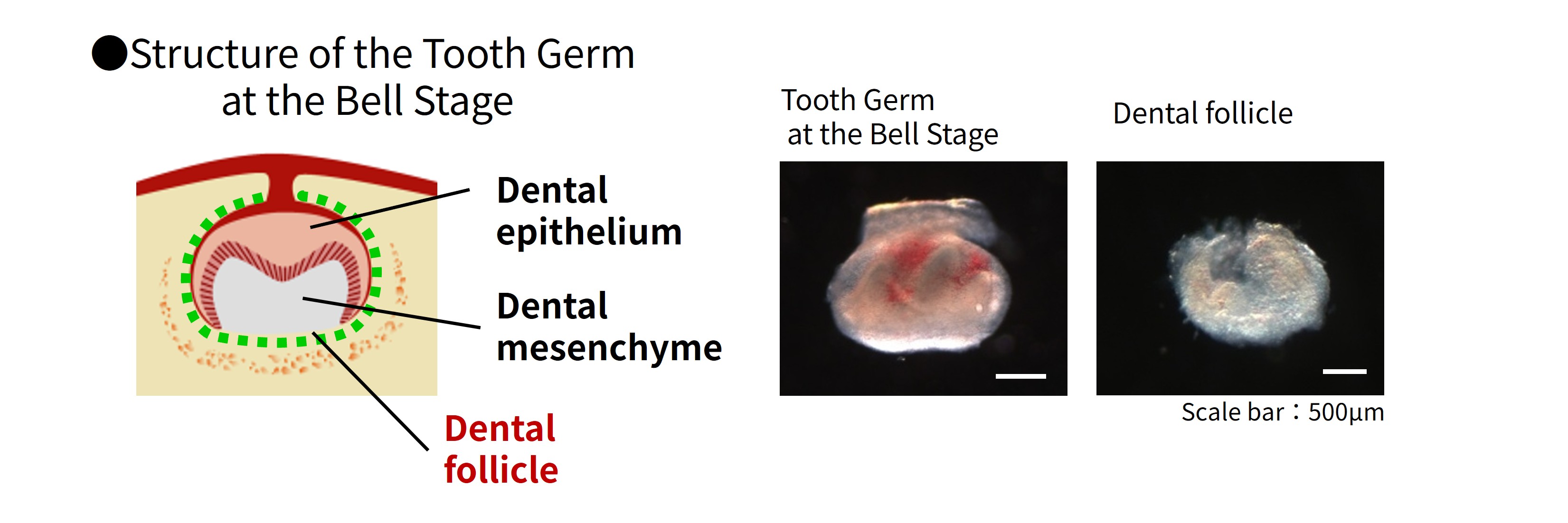
Teeth develop from a tooth germ induced during the fetal stage. Surrounding this developing tooth germ is the Dental follicle, a tissue destined to differentiate into periodontal tissues—namely Cementum, Periodontal ligament, and Alveolar bone (Chapter 1).
To induce periodontal tissue formation around the implant, we first utilized Dental follicle tissue. Because titanium implant surfaces are biologically inert and poorly support cell attachment, the implant surface was coated with a thin layer of hydroxyapatite (HA), which has been reported to promote cellular differentiation toward bone-forming lineages. The HA-coated implant was wrapped with Dental follicle tissue and transplanted into an extraction socket to evaluate whether periodontal ligament formation could be achieved.
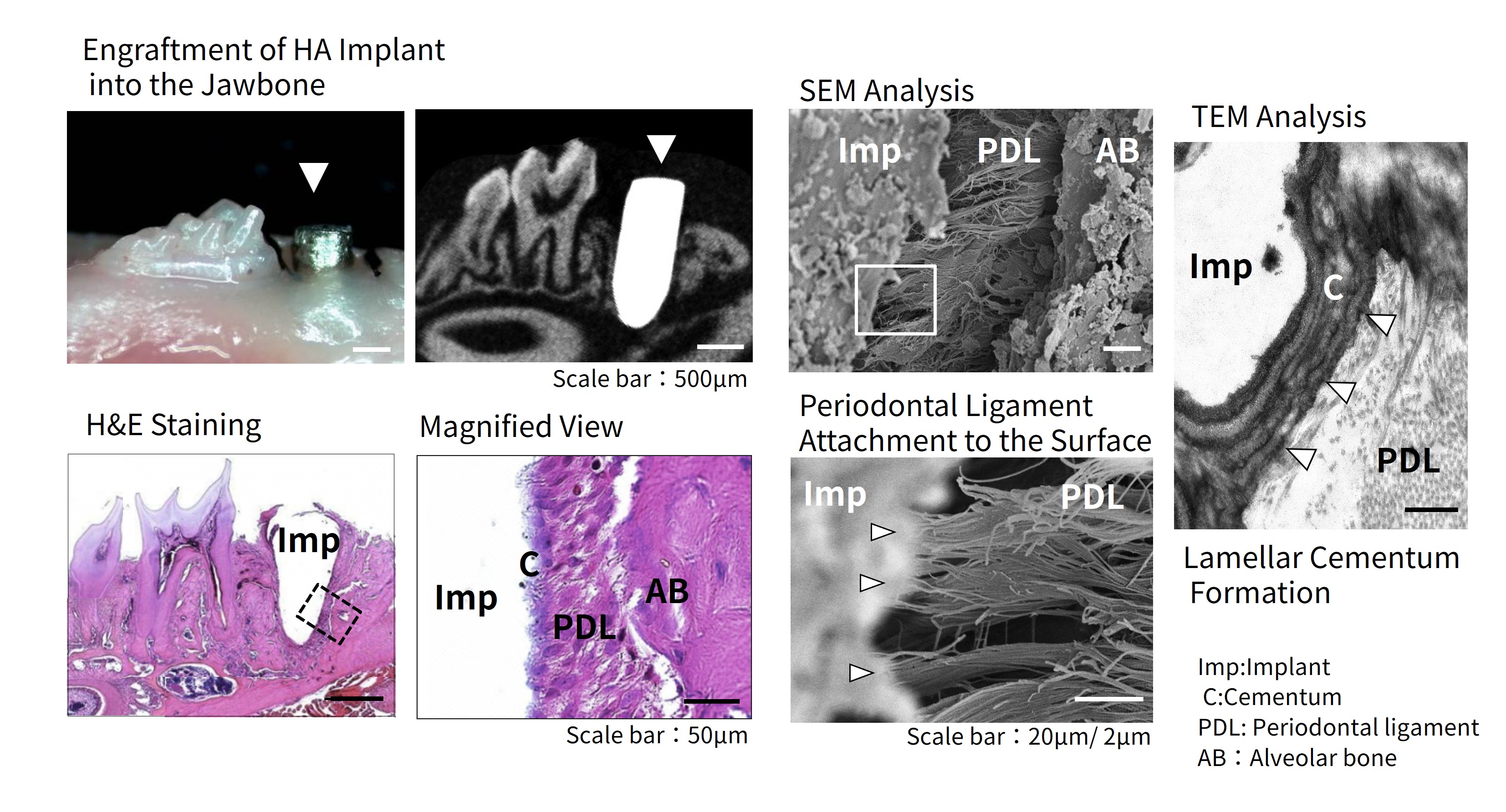
When HA implants alone were transplanted, conventional osseointegration, characteristic of an osseointegrated implant, was observed.
In contrast, transplantation of HA implants wrapped with Dental follicle tissue resulted in the orderly formation of periodontal tissues arranged sequentially from the implant surface outward: Cementum, Periodontal ligament, and Alveolar bone.
Ultrastructural analysis using electron microscopy revealed lamellar Cementum formation on the implant surface and insertion of periodontal ligament Sharpey’s fibers (Figure 2). These findings demonstrated that transplantation of HA implants combined with Dental follicle tissue enabled engraftment through periodontal tissues containing a functional periodontal ligament comparable to that of a Natural tooth.
Next, we examined whether implants endowed with a periodontal ligament possessed physiological periodontal function.
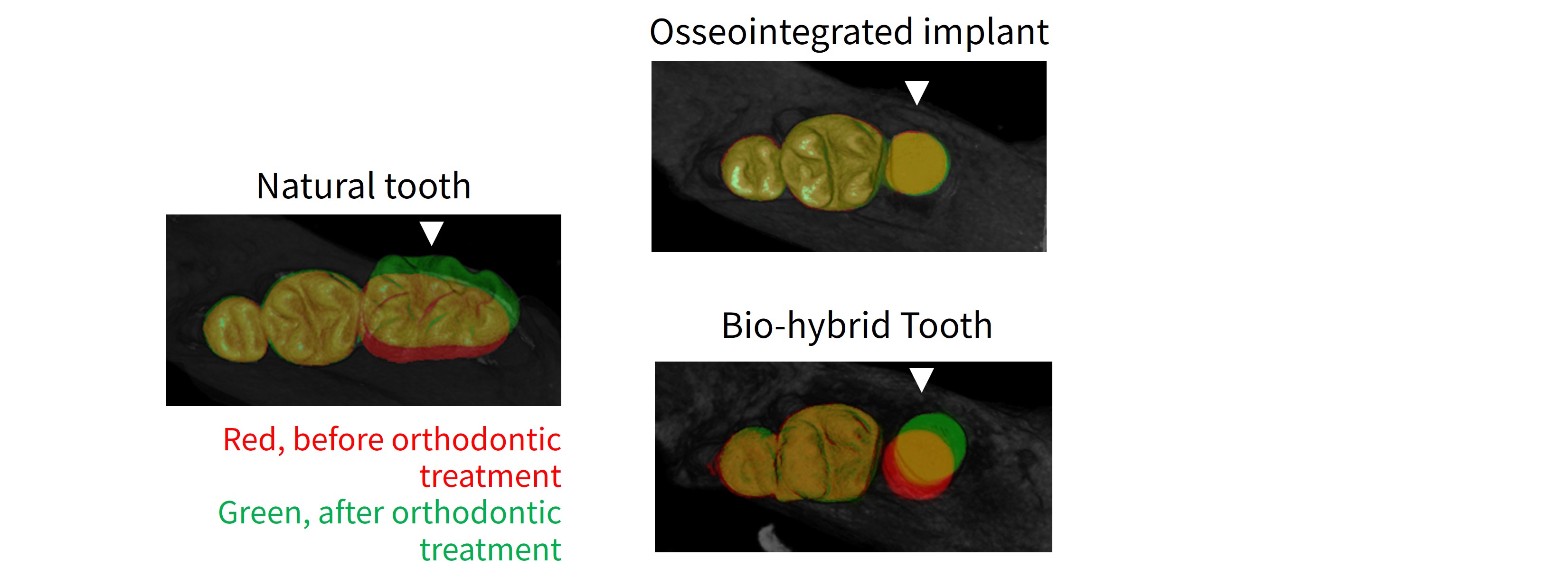
We first analyzed tooth movement induced by mechanical external force.
Conventional osseointegrated implants do not move under orthodontic force. In contrast, implants provided with a periodontal ligament exhibited time-dependent displacement in response to experimental orthodontic loading, similar to Natural teeth (Figure 3).
This movement was accompanied by physiological bone remodeling, characterized by localization of osteoclasts on the compression side and osteoblasts on the tension side. These results demonstrated that the regenerated periodontal ligament retained normal physiological function.
Teeth function as components of a functional occlusal system, forming neural networks connecting peripheral nerves in the craniofacial region with the central nervous system. These networks enable perception of occlusal force, tactile sensation, and nociceptive stimuli, thereby contributing to biological defense mechanisms (Chapter 1).
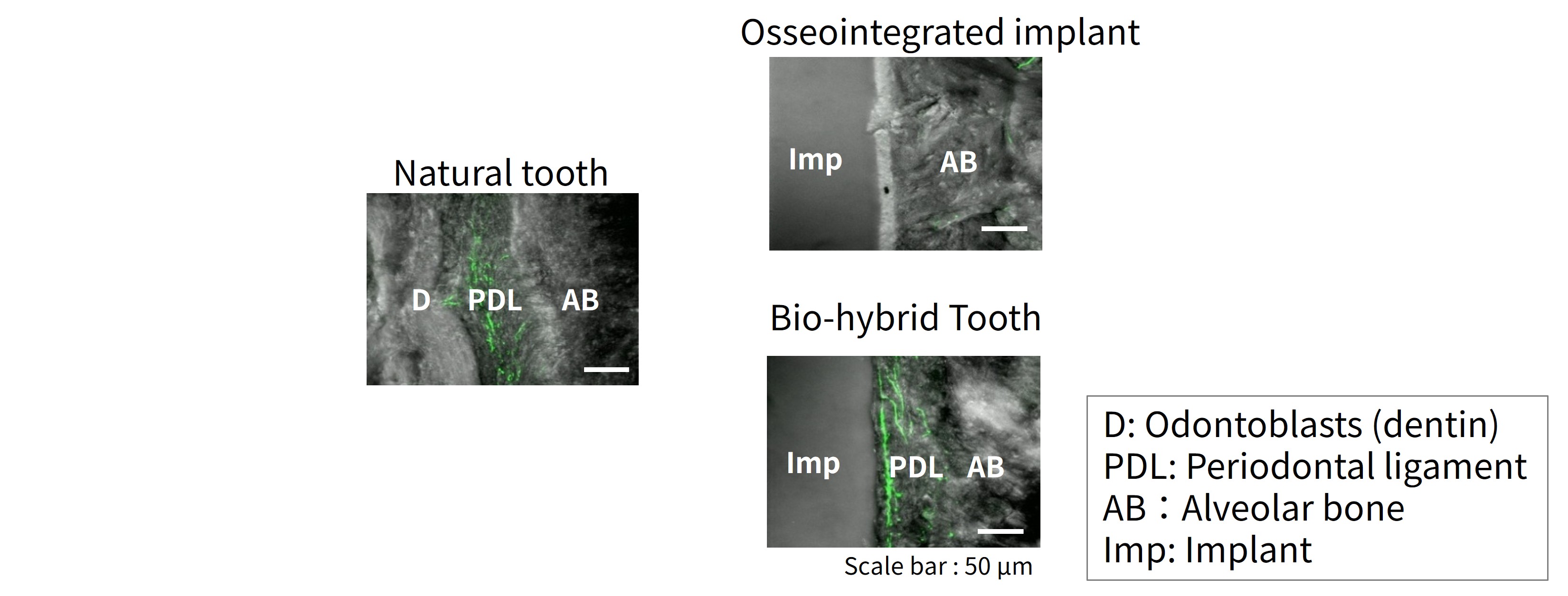
Because osseointegrated implants lack a periodontal ligament, regulation of occlusal force is limited, and excessive loading may result in mechanical complications.
In contrast, peripheral nerves were identified within the regenerated periodontal ligament surrounding the biohybrid implant (Figure 4). Furthermore, experimental orthodontic stimulation applied to these nerves was transmitted to the medulla oblongata, demonstrating that periodontal ligament–equipped implants possessed neural connectivity with the central nervous system and restored sensory perception during mastication.
These fundamental mouse studies demonstrated that placement of fetal-derived Dental follicle tissue around implant fixtures and transplantation into tooth-loss sites enables construction of implants possessing a functional periodontal ligament.
This technology represents a next-generation functional implant—namely a biohybrid implant—that restores periodontal ligament function, a major limitation of current oral implant therapy, thereby recovering physiological functions equivalent to those of a Natural tooth and reestablishing the functional occlusal system (Chapter 1).
However, because this stage relied on fetal-derived tissues, further technological development is required to achieve clinical application in humans using adult biological environments and cell sources, including Epithelial stem cells and Mesenchymal stem cells (MSCs).
Accordingly, we restarted our research program using large-animal models to advance toward clinical translation and human therapeutic application.
