Chapter
5 OrganTech's Challenge (2-2)
- Integrating Implants with the Body Through the Periodontal Ligament
5 OrganTech's Challenge (2-2)
- Integrating Implants with the Body Through the Periodontal Ligament
Last updated: March 27, 2026

Miho Ogawa, Ph.D. Director, CTO
Ph.D. in Science from Tokyo University of Science Graduate School. After working at Otsuka Holdings and RIKEN, became Director and CTO of OrganTech Inc. Promotes research, development, and commercialization in regenerative medicine and organ induction. Recipient of the Japan Sjogren's Syndrome Society Award and the Economist Future Award 2023 SDGs Division. View full profile >
Ph.D. in Science from Tokyo University of Science Graduate School. After working at Otsuka Holdings and RIKEN, became Director and CTO of OrganTech Inc. Promotes research, development, and commercialization in regenerative medicine and organ induction. Recipient of the Japan Sjogren's Syndrome Society Award and the Economist Future Award 2023 SDGs Division. View full profile >
Can the Periodontal Ligament Be Recreated Around an Implant?
Conventional implant treatment stabilizes an implant by allowing it to bond directly with the jawbone. This process, known as an osseointegrated implant, has greatly advanced dental treatment. However, unlike a natural tooth, these implants do not contain a periodontal ligament, an important tissue normally found around natural teeth.
Many studies have attempted to regenerate this ligament using different techniques, but recreating complete periodontal tissues—including cementum, the periodontal ligament, and alveolar bone—with the same structure as a natural tooth had not previously been achieved.
For this reason, OrganTech, Inc. began research in 2009 from the perspectives of developmental biology and regenerative medicine to develop an implant that, like a natural tooth, connects to the bone through the periodontal ligament.
Many studies have attempted to regenerate this ligament using different techniques, but recreating complete periodontal tissues—including cementum, the periodontal ligament, and alveolar bone—with the same structure as a natural tooth had not previously been achieved.
For this reason, OrganTech, Inc. began research in 2009 from the perspectives of developmental biology and regenerative medicine to develop an implant that, like a natural tooth, connects to the bone through the periodontal ligament.
Focusing on the Dental Follicle — the Origin of Tooth-Supporting Tissues
Teeth develop during fetal growth from a structure called a tooth germ.
Surrounding this tooth germ is a tissue known as the dental follicle.
The dental follicle later develops into the tissues that support teeth:
・Cementum
・Periodontal ligament
・Alveolar bone
In simple terms, the dental follicle is a collection of cells that becomes the foundation of tooth-supporting tissues.
We therefore investigated whether using dental follicle tissue could allow a periodontal ligament to form around an implant.
Surrounding this tooth germ is a tissue known as the dental follicle.
The dental follicle later develops into the tissues that support teeth:
・Cementum
・Periodontal ligament
・Alveolar bone
In simple terms, the dental follicle is a collection of cells that becomes the foundation of tooth-supporting tissues.
We therefore investigated whether using dental follicle tissue could allow a periodontal ligament to form around an implant.
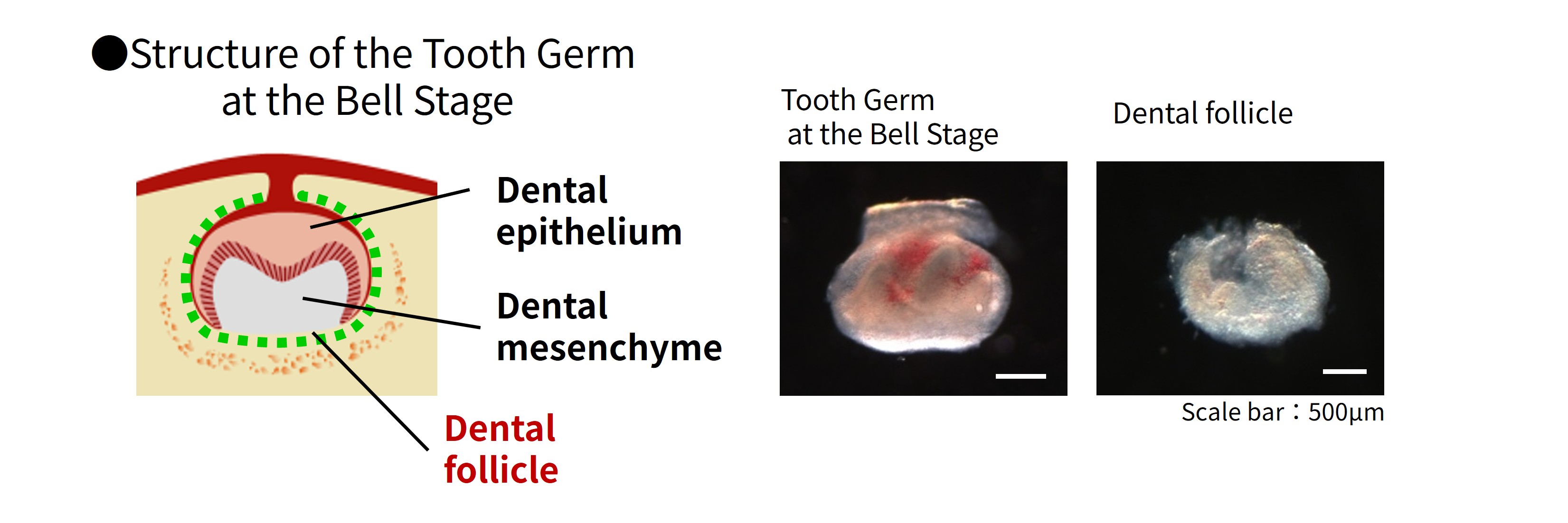
Figure 1 Bell-stage tooth germ and Dental follicle tissue
Dental implants are typically made of titanium metal, but cells do not easily attach to titanium surfaces. To solve this problem, we coated the implant surface with a thin layer of hydroxyapatite (HA), a material highly compatible with bone.
Dental follicle tissue was wrapped around this HA-coated implant and transplanted into a tooth extraction site to examine whether a periodontal ligament could form.
Dental follicle tissue was wrapped around this HA-coated implant and transplanted into a tooth extraction site to examine whether a periodontal ligament could form.
Formation of Periodontal Tissues Around the Implant
The experimental results were very encouraging.
When only the HA implant was transplanted, it fused directly with bone, just like conventional implants.
However, when dental follicle tissue was added, tissues formed around the implant in the same order seen in a natural tooth:
・Cementum
・Periodontal ligament
・Alveolar bone
This meant that complete periodontal tissues had developed around the implant.
Detailed observation using electron microscopy further confirmed that:
・Cementum formed on the implant surface
・Collagen fibers of the periodontal ligament (Sharpey’s fibers) inserted into the surface
In other words, the implant was connected to bone through a periodontal ligament rather than direct bone fusion.
When only the HA implant was transplanted, it fused directly with bone, just like conventional implants.
However, when dental follicle tissue was added, tissues formed around the implant in the same order seen in a natural tooth:
・Cementum
・Periodontal ligament
・Alveolar bone
This meant that complete periodontal tissues had developed around the implant.
Detailed observation using electron microscopy further confirmed that:
・Cementum formed on the implant surface
・Collagen fibers of the periodontal ligament (Sharpey’s fibers) inserted into the surface
In other words, the implant was connected to bone through a periodontal ligament rather than direct bone fusion.
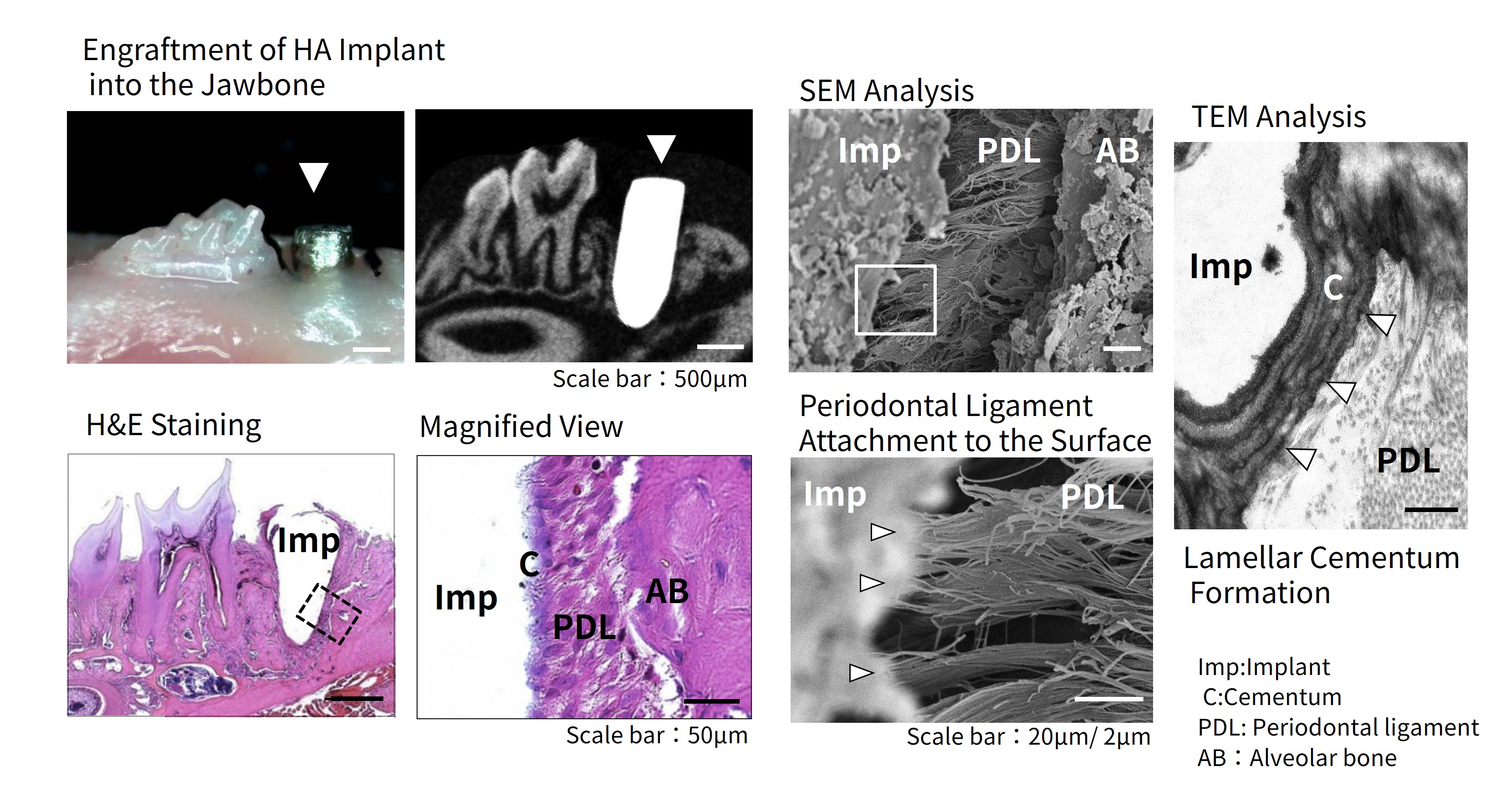
Figure 2 Evaluation of tissue integration around HA implants (HE staining, SEM/TEM analysis)
Does the Periodontal Ligament Function Properly?
Next, we investigated whether this implant actually worked like a natural periodontal ligament.
In natural teeth, orthodontic force slowly moves teeth because the periodontal ligament allows bone remodeling.
By contrast, an osseointegrated implant does not move because it is directly fused to bone.
Remarkably, implants provided with a periodontal ligament moved gradually in response to orthodontic force, just like natural teeth.
This demonstrated that normal bone remodeling was occurring and that the regenerated periodontal ligament was functioning biologically.
In natural teeth, orthodontic force slowly moves teeth because the periodontal ligament allows bone remodeling.
By contrast, an osseointegrated implant does not move because it is directly fused to bone.
Remarkably, implants provided with a periodontal ligament moved gradually in response to orthodontic force, just like natural teeth.
This demonstrated that normal bone remodeling was occurring and that the regenerated periodontal ligament was functioning biologically.
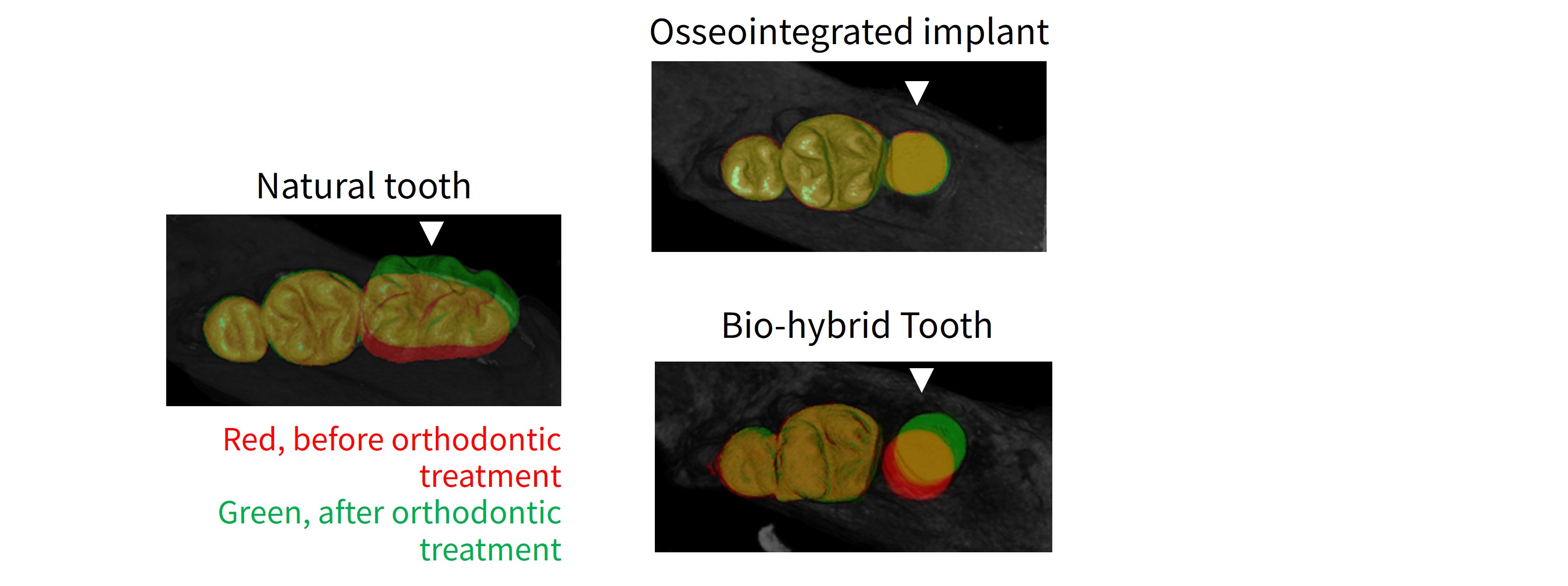
Figure 3 Tooth movement induced by orthodontic force
Recovery of the Sense of Biting
Another essential function of teeth is the ability to sense biting force.
In natural teeth, nerves located within the periodontal ligament detect pressure and stimulation and transmit this information to the brain through blood vessels and nerves.
Because conventional osseointegrated implants lack a periodontal ligament, fine control of biting force can be difficult.
Examination of the ligament-equipped implants revealed that peripheral nerve fibers had grown into the regenerated periodontal ligament. When these nerves were stimulated experimentally, signals were transmitted to the brainstem.
This suggests that the implant may restore sensory function—the ability to feel biting pressure.
In natural teeth, nerves located within the periodontal ligament detect pressure and stimulation and transmit this information to the brain through blood vessels and nerves.
Because conventional osseointegrated implants lack a periodontal ligament, fine control of biting force can be difficult.
Examination of the ligament-equipped implants revealed that peripheral nerve fibers had grown into the regenerated periodontal ligament. When these nerves were stimulated experimentally, signals were transmitted to the brainstem.
This suggests that the implant may restore sensory function—the ability to feel biting pressure.
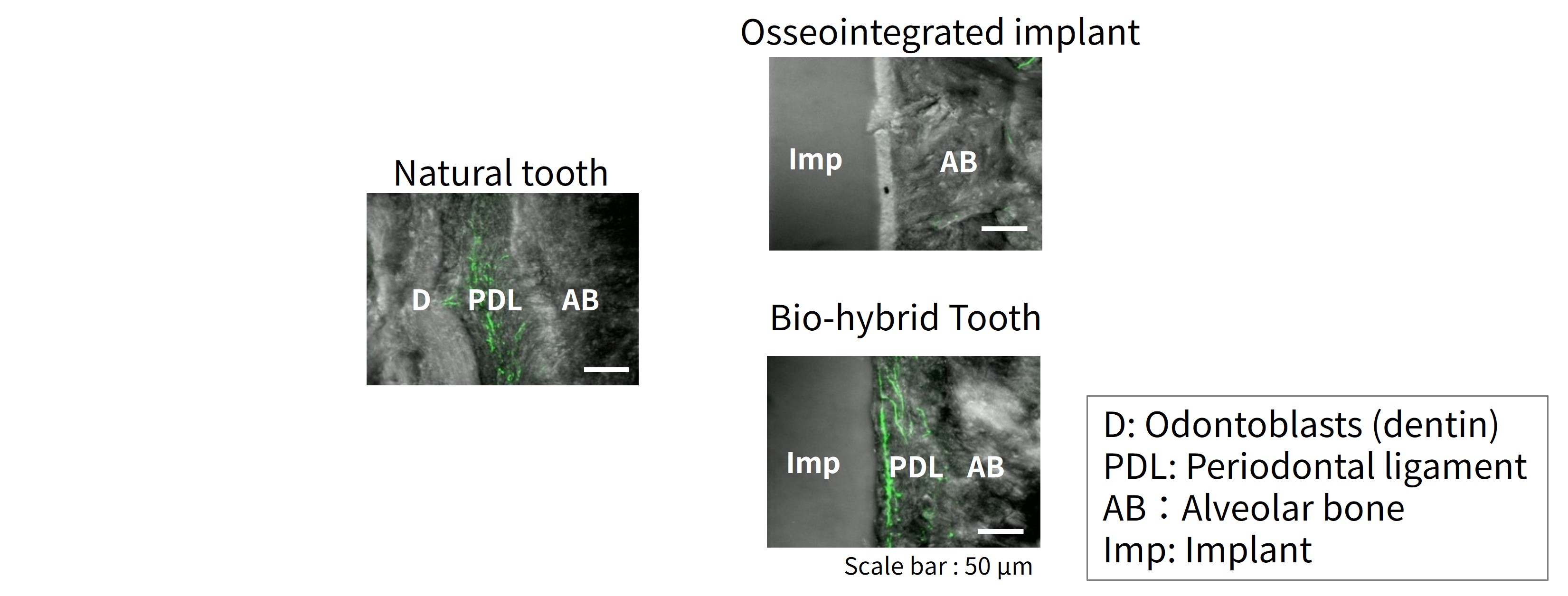
Figure 4 Distribution of peripheral nerve fibers within regenerated periodontal ligament (immunofluorescence staining)
Toward Next-Generation Dental Implants
These findings demonstrate the possibility of creating implants that connect to bone through a periodontal ligament.
Such technology could overcome current limitations of implant treatment by restoring:
・regulation of biting force
・natural physiological tooth function
This approach represents a next-generation functional implant and may lead toward therapies similar to a bioengineered tooth.
However, the present study used fetal-derived dental follicle tissue. For clinical application in humans, new technologies using cells already present in the adult body—such as epithelial stem cells and mesenchymal stem cells (MSCs)—must be established.
In Chapter 1, we introduced the basic concept.
In Chapter 6, we will introduce studies using large-animal models aimed at clinical application in humans.
Such technology could overcome current limitations of implant treatment by restoring:
・regulation of biting force
・natural physiological tooth function
This approach represents a next-generation functional implant and may lead toward therapies similar to a bioengineered tooth.
However, the present study used fetal-derived dental follicle tissue. For clinical application in humans, new technologies using cells already present in the adult body—such as epithelial stem cells and mesenchymal stem cells (MSCs)—must be established.
In Chapter 1, we introduced the basic concept.
In Chapter 6, we will introduce studies using large-animal models aimed at clinical application in humans.
* This article reflects research and development-stage information as of March 27, 2026, and does not represent finalized medical procedures or products.
